Do I Need a Third-Party HRA Administrator?

Do I Need a Third-Party HRA Administrator?
A Health Reimbursement Arrangement (HRA) — now under the Custom Health Option and Individual Care Expense (CHOICE) Arrangement umbrella — is an employer-sponsored health benefit that prioritizes cost predictability.
It allows employers to set fixed reimbursement allowances for eligible employees, which can be used to pay insurance premiums as well as qualified, out-of-pocket medical expenses.
While HRAs sound simple on paper, they still come with administrative burdens.
This leads to the question: Do you need a Third-Party Administrator (TPA) for an HRA?
First, let's do a quick review of the facts:
What is a TPA?
A TPA is an external individual or team responsible for setting up, managing, and enforcing their client's health plan. In a broader sense, this could pertain to provider contract negotiations, stop-loss insurance coordination, delivering managed care, COBRA administration, and fiduciary oversight.
But when it comes to HRAs, their role revolves around three critical objectives:
- Preparing HRA Documentation — One of the biggest value propositions of having a TPA is that you don't have to deal with compliance-related headaches, and that includes creating the necessary plan documentation. This includes the complete HRA Summary Plan Document (SPD) and reporting forms (e.g., 1094-B, 1095B, 1094-C, 1095-C, and Form 720).
- Verifying Reimbursement Claims — TPAs will also be in charge of accepting and reviewing reimbursement requests from covered individuals. Aside from validating submitted receipts, they'll also inspect out-of-pocket expenses if they're covered under the IRS-approved list of medical expenses.
- Processing Reimbursements — Thirdly, TPAs will be tasked to handle the tax-free movement of funds between the employer and employee. The goal here, of course, is to lift the HRA-related administrative burdens from employers while making sure transactions are done on time.
How Much Does a TPA Cost?
The most accurate answer is also the shortest: it depends.
There's a slew of variables that go into a TPA's pricing, including the number of participants, HRA type, and any additional non-core services.
Looking at the overall cost structure, TPAs often break it down to the following fees:
- Setup Fee — The upfront cost of setting up your HRA, ranging anywhere from $150 to upwards of $1,500. This can be waived under circumstances like the use of bundled services, promotional offers, and volume-related contract negotiations.
- Per Employee Per Month Fee (PEPM) — The PEPM fee refers to the set amount you pay each month for every participant in your HRA. This can range from a small $2 to over $30 per employee per month.
- Base Annual or Platform Fees — Most TPAs also charge a base administration fee, which can be billed on a monthly or annual basis. Similar to setup fees, TPAs can also waive platform fees at their discretion.
- Add-On Fees — Lastly, TPAs may also charge for extra services like COBRA integration, annual report filings, and plan amendments. Just remember that it's possible to land a TPA that automates or handles these tasks for free.
Add a clear statement that QSEHRA is limited to employers with 2–50 employees, has different regulatory requirements, and is NOT the same as ICHRA; ensure the table and discussion separately address each arrangement. and business size:
Company Size | QSEHRA | ICHRA |
1-10 employees | $50-$300 per month | $20-$300 per month |
10-20 employees | $250-$550 per month | $200-$600 per month |
20-49 employees | $450-$1,200+ per month | $400-$1,200+ per month |
50+ employees | Not eligible for QSEHRA | $1,000-$5,000+ per month |
Benefits of a TPA for an HRA
Apart from administrative relief and pain-free compliance, TPAs will also help you design cost-effective and sustainable HRA plans. They also help bring down "hidden" operational costs of healthcare — along with the risks involved with mismanagement — through automation and expert oversight.
Most modern TPAs offer web portals that simplify reimbursement requests, fund tracking, and reporting, making the process seamless for employers and employees.
Are TPAs Mandatory for HRAs?
No, businesses don't need to use a TPA to offer HRAs to their employees.
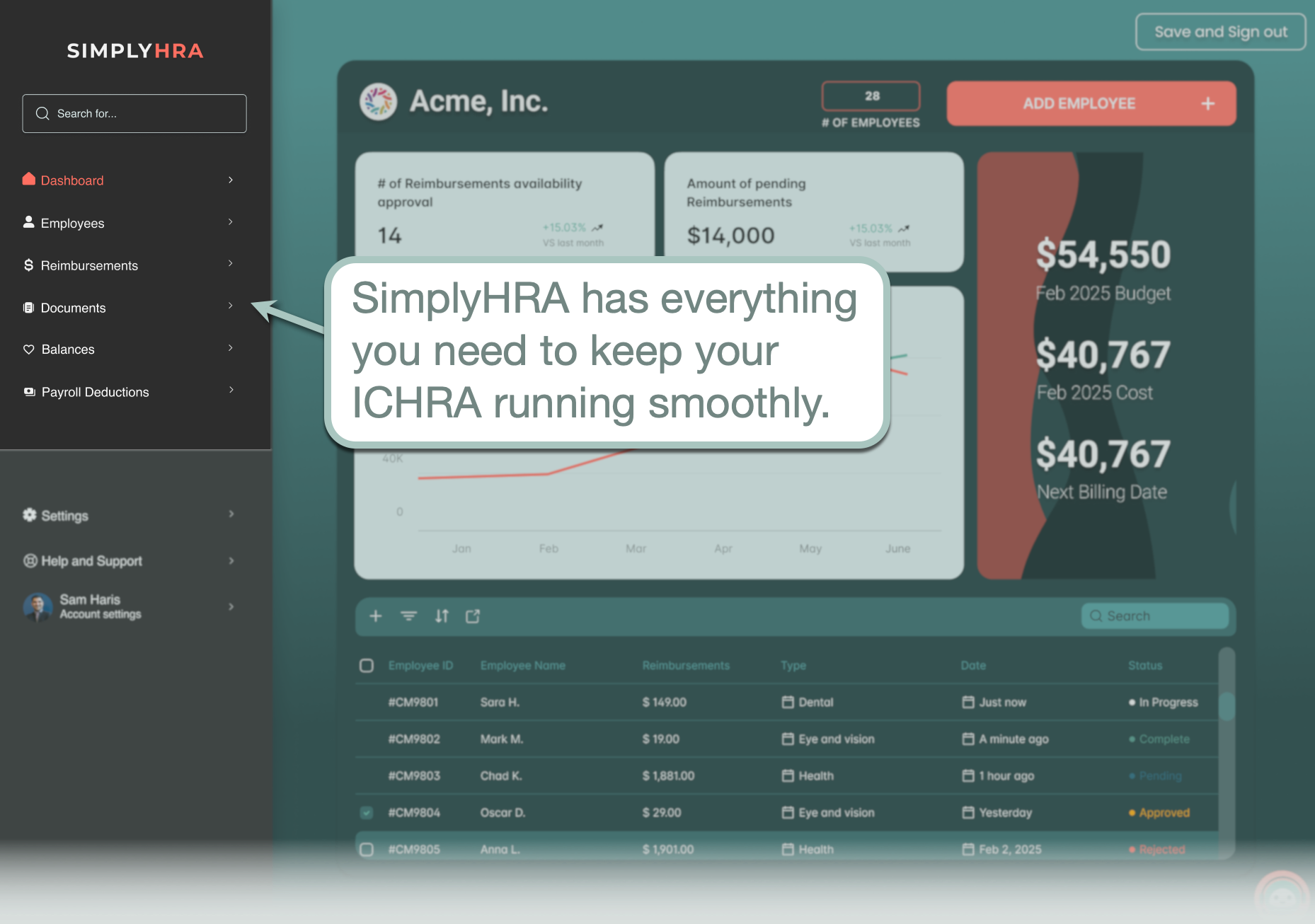
It's more than possible for employers to self-administer their HRA plans either manually or through specialized software like SimplyHRA.
For starters, SimplyHRA is a visual benefits platform specifically designed for ICHRA (short for "Individual Coverage Health Reimbursement Arrangement"). This makes it easier, more manageable, and more cost-effective for employers to self-manage the entire ICHRA pipeline — from employee onboarding to reimbursement processing.
Here's more good news: Choosing a self-administration software doesn't mean missing out on the compliance and convenience benefits that come with a TPA.
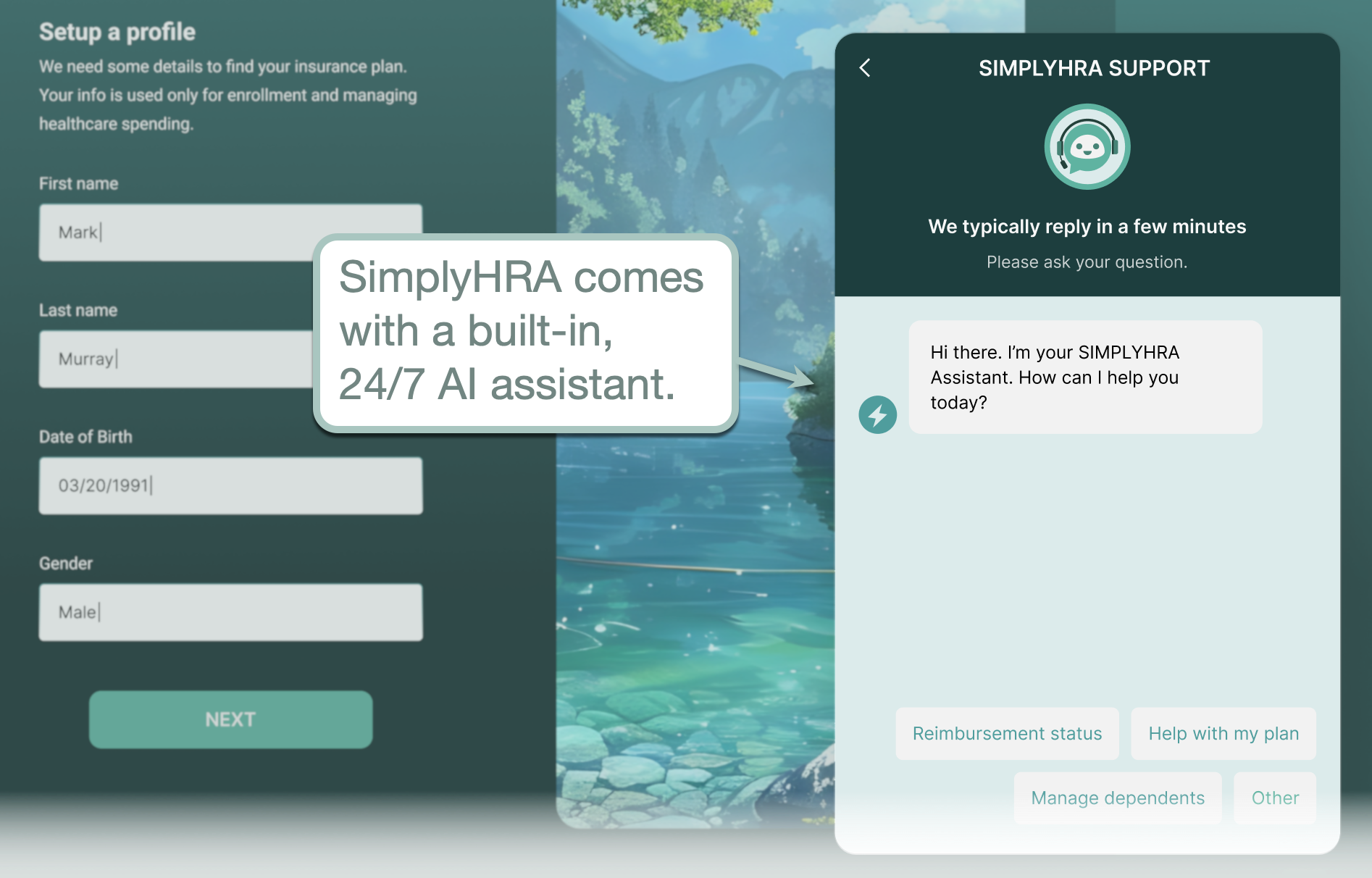
Not only will SimplyHRA handle all tax and compliance-related paperwork, it also comes with a built-in AI assistant to streamline employee training. It can provide reimbursement status updates, direct users to the right page, or answer pretty much any question related to ICHRA.
Got your attention?
Click here to schedule a personalized demo and see SimplyHRA in action.
Frequently Asked Questions
What's the Difference Between TPAs and ASOs?
An Administrative Services Only (ASO) is a part of a bigger health insurance carrier designed to provide administrative relief and compliance assistance. But unlike a more flexible TPA that can provide tailored health plans, ASOs can only offer standardized benefits tied to the carrier they're under.
What's the Difference Between a TPA and a Benefits Platform?
There are plenty of overlaps between a TPA and a benefits platform, specifically modern ones like SimplyHRA — from done-for-you compliance to automated reimbursement workflows. Just bear in mind that not all benefits platforms will shoulder all the administrative and compliance responsibilities that come with offering HRAs.
Is a TPA for HRA Worth It?
Using a TPA is generally a good move since they unlock ease of administration, simplified compliance, and better employee satisfaction through a more streamlined reimbursement process. But if you're willing to do a little bit of administrative work in exchange for more control over your HRA, it's often better and more prudent to go with a benefits administration platform.
Get Started with ICHRA Today
Curious to see what a winning ICHRA plan looks like?
With SimplyHRA, you can sidestep the stumbling blocks associated with ICHRA and get straight to offering cost-effective, flexible, and accessible health plans to your employees.
It's everything good about ICHRA — but without the downsides and bottlenecks.
Schedule a personal demo here to learn more.
Related blogs

Is ICHRA a Good Fit in 2026? 7 Scenarios for Employers

HRA vs HSA Plans 2026: Differences, Limits & How to Choose